Get Healthy!
- Posted February 16, 2022
Giving the Heart a Push to Help Ease Long COVID
Could a therapy used to treat chest pain ease the debilitating symptoms of long COVID?
Yes, claims a small but promising study that found it helped ease fatigue, shortness of breath and other symptoms in people who can't shake side effects that haunt them long after their original coronavirus infection.
As many as 50% of people who recover from COVID-19 may experience a constellation of such symptoms, and there's not much that doctors can do for these patients because long COVID is such a new entity.
Exactly why some people develop long COVID and others don't isn't fully understood yet, but researchers suspect that endothelial dysfunction - which occurs when large blood vessels on the heart's surface constrict instead of dilate - may play a role, explained study author Sachin Shah.
Enter enhanced external counterpulsation (EECP), said Shah, chief scientific officer at Flow Therapy, a nationwide EECP provider based in Fort Worth, Texas.
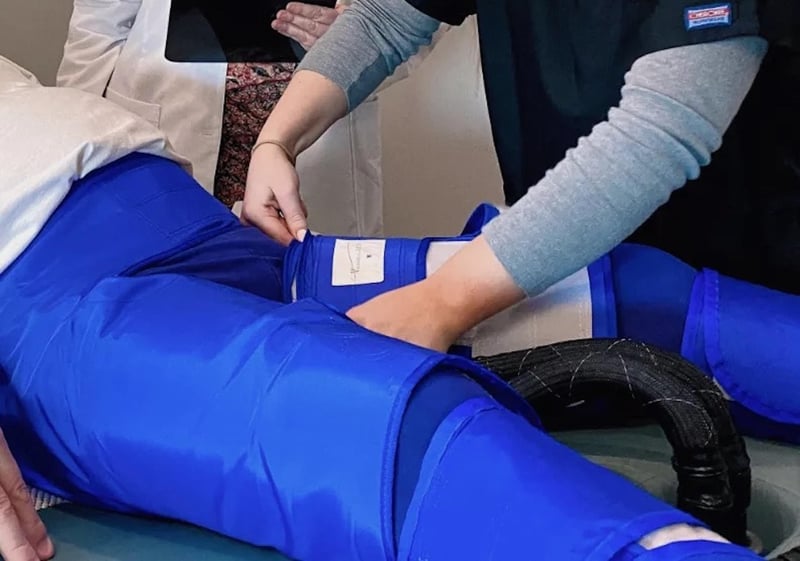
Folks who undergo EECP are fitted with three sets of cuffs on their calves, thighs and lower hips. These cuffs are inflated sequentially, from the calves up to the hips, when the heart is at rest. This action pushes oxygen-rich blood throughout the heart and to the rest of the body, and stimulates the formation of small branches of blood vessels to bypass narrowed arteries, he explained.
"The increased flow to the heart helps develop small vessels called collaterals that are a natural defense to heart disease, and the increase of blood flow throughout the body increases the overall health of the entire cardiovascular system by increasing the dilation and reducing inflammation of the blood vessels," Shah said.
Treatment with EECP lasts one hour, and people may need up to 35 sessions over seven weeks for maximum results, he said. The cost - roughly $9,500 for 35 treatments at Flow Therapy - may not be covered by insurance for treating long COVID, but Shah said he is working with insurers to get them to foot the bill.
The new study included 33 people with long COVID (average age 54), including 18 patients with no history of heart disease, who underwent EECP.
Everyone showed improvements in fatigue, breathing difficulties and chest discomfort after undergoing 15 to 35 hours of EECP therapy, even in those without a history of heart disease, the study showed. EECP benefits can last several years for people with angina, but more research is needed to see how long these improvements might last for people with long COVID, Shah said.
"Long COVID patients with and without coronary artery disease [CAD] who are suffering from marked limitations with ordinary activity in the form of fatigue, shortness of breath, chest discomfort and/or brain fog are the ideal candidates," Shah said. "Of course, in patients without long COVID having symptomatic CAD, EECP can do wonders for them."
The study was presented at a virtual meeting of the American College of Cardiology, held from Feb. 16 to 19. Findings presented at medical meetings should be considered preliminary until published in a peer-reviewed journal.
"This is an interesting concept that needs to be studied more," said Dr. Erica Spatz. She is an associate professor of cardiology at the Yale School of Medicine in New Haven, Conn., and a member of the ACC Science & Quality Committee.
"We do think there is a component of endothelial dysfunction with long COVID that may cause chest pain and exercise intolerance that is not detected on standard imaging tests," said Spatz. Making a diagnosis of endothelial dysfunction requires invasive testing, she added.
While it does seem to show promise for treating long-COVID, EECP is not widely available at this time, she noted.
More information
Find out what the U.S. National Institutes of Health is doing to better understand long COVID.
SOURCES: Sachin Shah, PharmD, chief scientific officer, Flow Therapy, Fort Worth, Texas; Erica Spatz, MD, associate professor, cardiology, Yale School of Medicine, New Haven, Conn., member, ACC Science & Quality Committee; American College of Cardiology's Cardiovascular Summit, virtual meeting, Feb. 16 to 19, 2022
